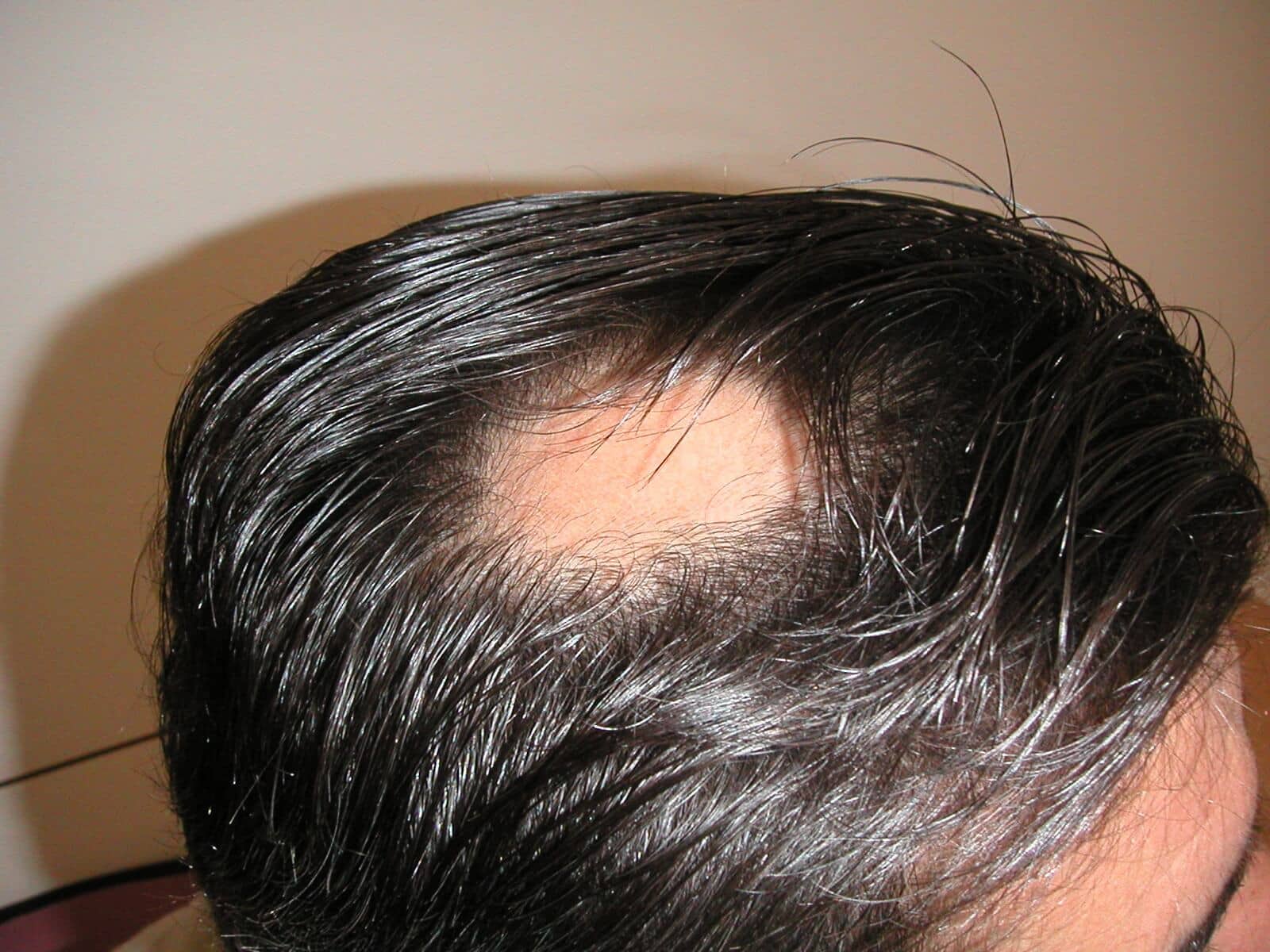
Using both patient and physician interviews, agreement was reached across these stakeholders that an absolute SALT score ≤ 20, that is, less than or equal to 20% scalp hair loss, should be the therapeutic goal. Recently, an Investigator Global Assessment tool was developed to describe the severity spectrum for scalp hair loss. For example, S 4a of 75–95% is less than S 4b of 96–99% hair loss, but both categories lack a specific descriptor that is, should these groups be considered moderate-to-severe versus severe OR severe versus very severe OR very severe versus extreme? Without having interpretive labels, the SALT S categories do not establish a common lexicon for the severity spectrum across the patient population. 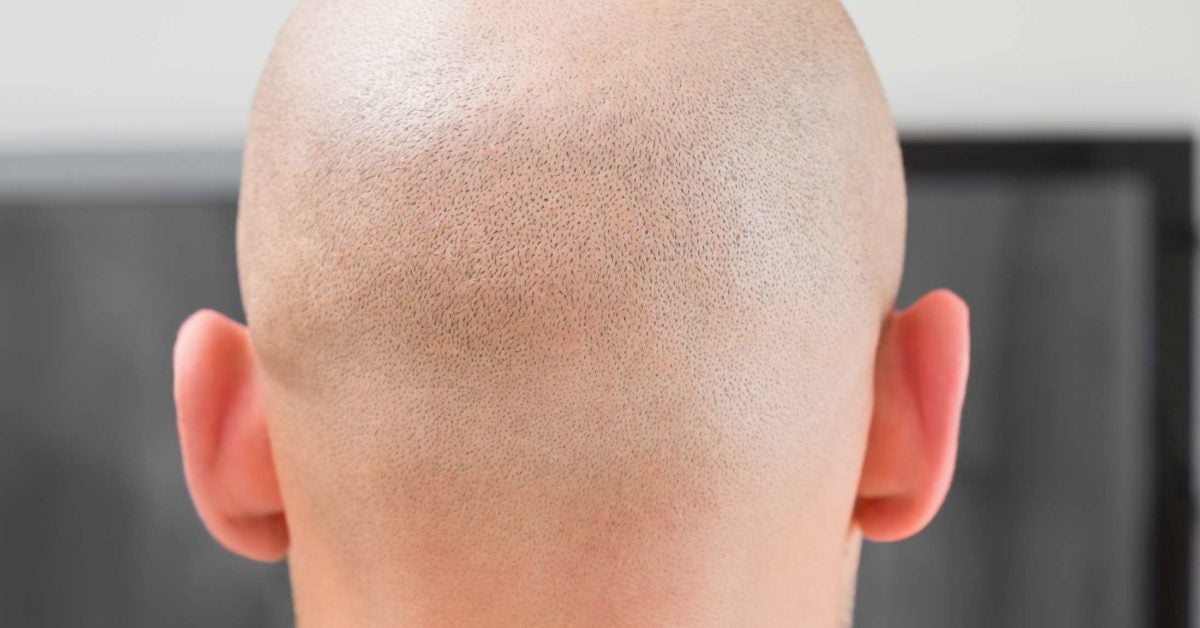
Ī limitation of the SALT is that the label for each category is ordinal without interpretation. In the Alopecia Areata Progression Index, the quantitative assessment of hair loss via the SALT is paired with indices of disease activity (hair pulling test and trichoscopy) to obtain a score that reflects activity, density, and extent of loss. Another variation of the SALT incorporates disease activity by quantifying density and shedding. The SALT II, based on the original SALT, delineates scalp surface area into 1% segments, allowing for more refined assessment for smaller patches of alopecia, and it is utilized for calculating the ALODEX score. The category S 4 was further subdivided into S 4a = 75–95% hair loss and S 4b = 96–99% hair loss, with the rationale that S 4b has prognostically lower probability for regrowth than S 4a. In its initial development, severity was classified as S 0 = no hair loss S 1 = 1–24% hair loss S 2 = 25–49% hair loss S 3 = 50–74% hair loss S 4 = 75–99% hair loss and S 5 = 100% hair loss. The Severity of Alopecia Tool (SALT) was developed to standardize the quantification of hair loss across the different quadrants of the head, and is commonly used for quantifying amount of scalp hair loss in clinical trials. In more recent years, disease severity in AA has been anchored in the extent of total scalp hair loss. Although their recommendation was to combine the AA prehypertensive type with the AA common type, they recognized that the overall validity of the groupings was poor, given that patients presented with overlapping features or that the groupings excluded consideration of other potentially relevant prognostic factors, such as family history. 
through analyses of 356 patients who were grouped according to age and chronicity. Īn attempt to replicate these groupings was undertaken by Sharma et al. Comparing these groupings, she then observed differences in comorbidities to develop a four-category system: AA common (single patches that spontaneously regrow), AA prehypertensive (recurrent small patches and predisposition for hypertension), AA autoimmune (persistent alopecia with associated autoimmune conditions), and AA atopic (persistent alopecia with atopic comorbidity). Using the course (pattern and persistence over time) as the external criterion, she based groupings primarily on duration of episode and onset of the disease. Subsequently, she reviewed the clinical history and course of 1989 patients who were treated within the skin clinic at Kyoto University over an 18-year period. However, Ikeda (1965) proposed that this system was inadequate because it did not account for the course of the illness. In 1902, Besnier classified AA into three types based on pattern of hair loss and inflammation: AA vulgaris, AA decalvans, and AA ophiasis.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
